
Many people wonder if gluten causes inflammation in everyone or just in people with gluten disorders. I’ll get to the bottom of this controversial topic. This post contains affiliate links. Please read my disclosures.
Gluten disorders are real and serious, and I hope you’re paying attention if you even have a passing thought that gluten might be behind your fill-in-the-blank ailment.
I’m not trying to scare you with such dramatic information, but I do think you deserve to know the truth.
Whether you have celiac disease or gluten sensitivity, or you simply enjoy eating gluten, a protein found in wheat, rye, barley, and sometimes oats, you need to read this article.
There is science-backed evidence to suggest that gluten may be damaging your body in more ways than you may realize. This damage is not just happening in people with celiac disease, but also it’s happening to all who eat gluten.
Is Gluten Bad For You?
I’m careful not to tell people that a specific food group is “bad” for them, however, if the evidence is clear, I can’t help but speak up.
We know, without a doubt, that consuming tobacco is “bad” for us, as is sugar, particularly in excess. These are widely accepted truths.
But what about gluten? Is gluten just trendy to give up like a passing celebrity fad (47 percent of people say gluten-free is just a fad, according to Mintel Research)? Or is gluten a real threat to human health?
And is gluten just bad for people with celiac disease? Could it be “bad” for people with gluten sensitivity too?
Celiac Disease
If you have celiac disease, yes, gluten is bad for you. In fact, gluten causes your immune system to attack your small intestine.
The small intestine is responsible for absorbing and distributing nutrients from the food you eat to the rest of your body. A damaged small intestine can lead to a slew of annoying symptoms, more disease, and eventually, may lead to your death.
Gluten should be avoided by people with celiac disease like the plague.
Gluten Intolerance
However, people with gluten intolerance, also known as non-celiac gluten sensitivity (NCGS), may wonder if gluten is no good for them even if it doesn’t cause an autoimmune reaction as devastating as the one caused by celiac disease.
A team of researchers from Italy shed light on this topic and found that those with gluten sensitivity possess high levels of a molecule called zonulin.
Before I can explain why zonulin matters, let me first explain what it is.
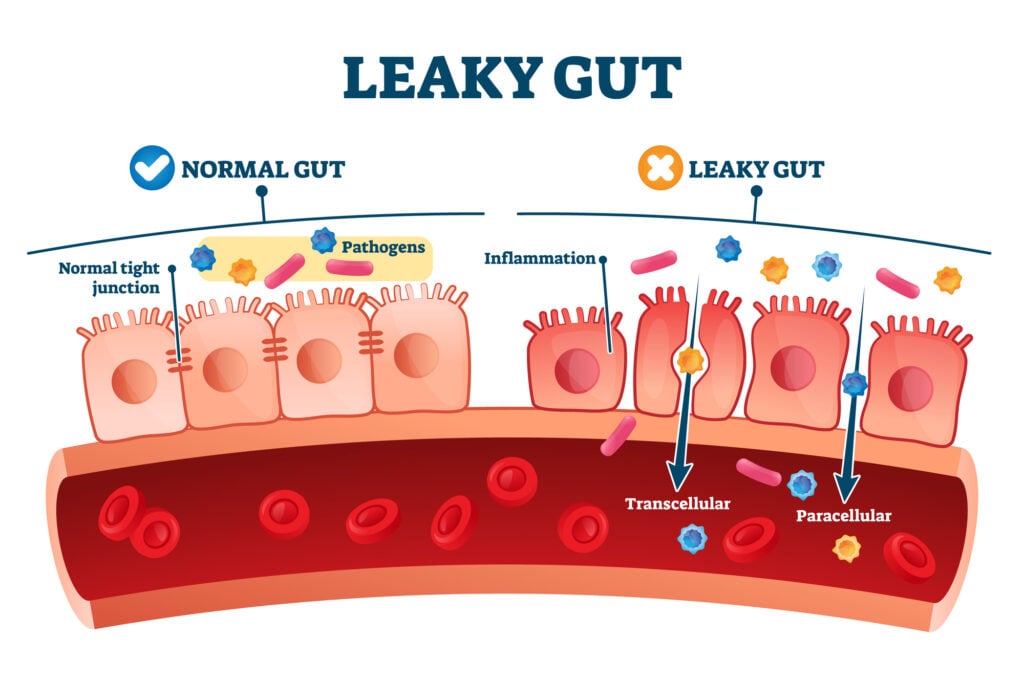
Zonulin is a protein that helps to regulate the “leakiness” of the gut. It’s responsible for opening and closing the spaces, known as the intestinal tight junctions (“tight junctions”), between the cells lining the digestive tract.
In healthy individuals, zonulin is triggered by harmful bacteria. Your body will produce high levels of zonulin to help trigger it to flush out the bacteria and bugs (i.e., diarrhea). Once your body rids of the pathogen, the tight junctions close and zonulin production subsides.
Leading celiac disease research doctor Alessio Fasano, also found high levels of zonulin in people with celiac disease, but he never researched people with gluten sensitivity. Do they have high zonulin levels as well?
Enter a team of Italian researchers. They set out to measure the levels of zonulin in (1) people with celiac disease, (2) people with irritable bowel syndrome (IBS), (3) people with gluten sensitivity, and (4) healthy volunteers.
Subjects with celiac disease and gluten sensitivity had high zonulin levels in their blood, while those with IBS displayed only elevated levels. Healthy volunteers experienced little or no increased zonulin levels.
Dr. Fasano told NPR, “No human being completely digests gluten. And in a small percentage of us, that undigested gluten triggers the release of zonulin.”
He added that many illnesses link back to the loss of barrier function in the gut, and figuring out how to regulate zonulin production could lead to better treatment options for people with celiac disease and gluten sensitivity.
Is Gluten “Bad” For Everyone?
Now that it’s easy to see how gluten is up to no good in people with celiac disease and gluten sensitivity, you might also wonder if it’s no good for the rest of the “healthy” population as well.
While healthy people do not have increased zonulin levels, something Dr. Fasano said stuck with me. He said, “No human being completely digests gluten.”
That means gluten is something we eat and excrete. It’s useless to us otherwise.
On top of that, additional research from Dr. Fasano suggests that a protein in gluten, gliadin, is not only indigestible but also that it causes inflammation – via intestinal permeability – in ALL who eat it.
The team of researchers looked at how four strains of wheat, including the two hybrid strains most commonly used in the U.S., as well as two ancient strains of wheat, impacted humans when consumed.
The researchers examined the following four subsets:
- Individuals recently diagnosed with celiac disease
- People with celiac disease on a gluten-free diet for at least one year (or longer)
- People with non-celiac gluten sensitivity
- People who had no known problem with gluten (without a known gluten disorder)
The researchers fed participants all strains of wheat and found that all four groups had the genes activated for intestinal permeability when exposed to wheat. This occurred in the subjects that had no known problem with gluten.
In other words, after all of the subjects ate wheat, all of their intestines showed signs of damage and inflammation. This damage came regardless if the person was on the gluten spectrum or not.
I first heard about this study from the leading gluten-sensitivity doctor in the world, Dr. Tom O’Bryan. He wrote about it in his book about autoimmunity, which I highly recommend. (Dr. O’Bryan wrote the foreword to my book, Dear Gluten, It’s Not Me, It’s You, and we collaborated to create the Gluten-Free Made Easy course.)
What Does This Mean?
Much research needs to be done to understand what all of this means.
The one thing we know for certain is that people with celiac disease and gluten sensitivity must avoid all gluten, even bits of gluten resulting from gluten cross-contamination.
For the rest of the population, researchers haven’t fully articulated what this research means. Humans have been eating gluten for thousands of years and have been fine, so why stop eating it now?
Dr. O’Bryan says in his book that every time anyone – not just someone with gluten sensitivity or celiac disease – eats gluten, it tears at their intestinal lining. He says the lining will heal and restore itself as it should, especially in healthy people.
However, he adds, at any sign of a weakened immune system and/or after being overworked day after day, meal after meal, the body will give out, and the small intestine lining fails to repair and restore fully. As a result, it will become leaky. It begins to show signs of continuous abuse. And when that happens, that’s when disease rears its ugly head.
Getting Tested for Celiac Disease and Gluten Sensitivity
The only way to know if you have celiac disease is to take a simple blood test that you can request from your doctor. You can also try this at-home celiac disease test kit, which is just as reliable. Read more about How to Get Tested for Celiac Disease.
Getting tested for non-celiac gluten sensitivity is a little more difficult, and there isn’t a consensus on how to do it.
That said, Dr. O’Bryan talks a lot about the Wheat Zoomer Test. This test evaluates you for celiac disease, non-celiac gluten sensitivity, non-gluten wheat sensitivity, and autoimmune processes triggered by gluten. It also can help you identify intestinal permeability (leaky gut syndrome) as well as bacterial lipopolysaccharides (LPS), which contribute to intestinal permeability.
Another test for gluten sensitivity is the Cyrex Array 3A test (Wheat/Gluten Proteome Reactivity & Autoimmunity), which you can order online or talk to your doctor about ordering for you.
You can read more about how to get tested for gluten intolerance in this article.
Research is Coming
While no one can definitively say that gluten is “bad” for all people, the research is showing that gluten is definitely up to no good for a large and growing percentage of the population.
And with explosive research suggesting that gluten causes intestinal permeability (leaky gut) in all who eat it, you can be certain that more research is coming to explore this phenomenon further.
In the meantime, those with celiac disease and gluten sensitivity should avoid sticky protein. For the rest of you, the research is still fledgling at best and does not justify a gluten-free diet for all.
Additional Reading
You might enjoy these articles too:
The food in the USA is allowed to have poison put on the wheat before it is harvested. The food industry lobbyist in DC have a lot of influence on those in congress and senate and with payoffs and kickbacks to those people, laws and processes are allowed that help the food industry make more money by using unsafe, unhealthy and BAD ingredients/ processes regardless if it is poison/unhealthy/damaging to “the people”.
If you can use organic grains/flour/products you may find you will feel better and not have all the terrible symptoms.
Until we take back our country and rein in the corruption in DC, the food in USA will be bad and unhealthy.
To all those saying this is an “agenda” or that it’s not bad for everyone, Look at the difference in our wheat today. The wheat in America contains More gluten and the gluten is water soluble, which it wasn’t in previous wheat strains. Our bodies are mostly water right? Do the math. Also, gluten looks like other organs/glands in the body like the brain and the thyroid. When your gut lining breaks down from the gluten and other bad proteins, it allows the gluten to cross into your bloodstream triggering an immune response. When your immune system sees it, it will tag it as a foreigner. Then bc it looks like the brain and thyroid, the body will attack these tissues, thinking it’s Also a foreigner.
Too many super healthy people all over the world who are eating bread for me to believe this ‘science’. I think it may be more a case of sensitivity to vital wheat gluten (vs natural gluten) as well as chemicals in processed food. People have survived on grains for hundreds of thousands of years. If gluten was bad, evolution would have corrected for it by now. Same with those decrying meat.
Thank you for sharing!!
@Elena – I lost weight eating gluten and gained eating gluten free, too. It’s amazing what happens when my body is actually able to ABSORB nutrients.
Gluten and dairy products have ripped up my colon. At my age the damage done irreparable. So please I beg of you be careful what you put in your mouth. I have autoimmune diseases and chronic inflammation. I have tried every diet nothing works. American food is unhealthy. Too late for me to move out of the country.
I’m so happy you figured it out. Cheers to your good health!!
I have MS, my symptoms were pretty bad but after being a gluten free for two years now I feel like I can do everything and more ? I will never eat gluten again my life!! I can walk better I can ride bike I feel amazing ??
Now I know I will live long and healthy life ❤️
From what I read of Dr. Gundry’s research – re Plant Paradox -, brown rice is not really that much better for a person than is whole wheat.
Agree that what works for one person may not work for another. I actually don’t think everyone needs to be gluten free but I do believe, based on research, that gluten is an inflammatory food.
You have celiac disease, so clearly, you’re biased. Vegans say this about animal products all the time. People in other countries eat gluten just fine. So please, stop letting your personal agenda cloud your judgement. People in the Swiss alps consume sourdough bread, and guess what? They have some of the healthiest teeth ever! I have actually lost weight eating gluten, and gained weight going gluten free. What works for one person may not work for another.
I also suspect that it’s more of a gmo/organophosphate issue. The Mediterranean has one of the healthiest populations in the world and they eat pasta or bread in limited amounts daily. Their strain of wheat is older so the gluten protein structure is different than the overbred stuff in the US. I would be hesitant to say all types are bad given the above evidence.
If you feel better, I’d say yes. Perhaps test for a gluten sensitivity – but I’d say you already intuitively know. Good luck!
My mother was a celiac. I have now been tested twice. Both came back negative. But I did feel better when I went gluten free. Should I stay gluten free?
The study showed all people had some sort of immune system response to gluten, however, so much research is still needed in this field to know what that means exactly. I’m hopeful we’ll have more research to better understand how gluten and other foods affect our bodies.
Sorry, unless people have an allergic reaction to foods that contain gluten, I’m not believing this. I think the problem is more about the refined & processed foods. I’m all about health, wellness, nutrition & healthy eating. Paleo, vegetarian, vegan.. and just good food, or even food in general.
I believe that people should eat what makes their body feel good! Thanks for the info though 🙂