
Traditionally, experts considered celiac disease a childhood condition, with symptoms appearing in the first few years of life. However, in the last decade, there has been a significant rise in the number of people being diagnosed with late-onset celiac disease or celiac that develops during adulthood. This post discusses why there’s a rise in late-onset celiac disease and the unique signs of celiac disease presenting in older patients. This post should not be construed as medical information. Discuss any changes to your diet or health with a doctor. Please see my disclosures.
Strong evidence today suggests that celiac disease can be diagnosed at any age, and the rate of late-onset celiac disease is skyrocketing among adult and elderly populations.
Celiac disease is a genetic autoimmune disease affecting one percent of the population. However, a 2017 study suggests the disorder affects closer to three percent of the population.
People with celiac disease suffer from varied symptoms, including classical gastrointestinal disorders like bloating, diarrhea, and gas, as well as nutritional deficiencies, bone density issues, joint pain, migraines, skin issues, and more.
Gluten, a protein found in wheat, rye, barley, and sometimes oats, triggers an immune system response in people with celiac disease. When a person with celiac disease eats gluten, their immune system mistakenly attacks the small intestine.
The small intestine is responsible for absorbing nutrients from food and distributing those nutrients to the rest of the body. Without a functioning small intestine, nutritional deficiencies ensue, and various maladies form as a result.

Why the Rise of Late-Onset Celiac Disease?
Some studies suggest the median age of a celiac disease diagnosis is 45 years old, with a “substantial portion” of patients being diagnosed after age 50.
In 1960, one study showed that barely four percent of newly diagnosed celiac disease patients were over 60. However, a 1994 study showed that 19 percent of patients were diagnosed at 60, and today, one-third of all new celiac patients are 65 and up.
Several theories explain why older patients are being diagnosed with celiac disease at increasing rates.
(1) Changes in the Gut Microbiome
The role of the gut microbiome cannot be overlooked when considering late-onset celiac disease. The collection of microorganisms that live in the digestive tract absolutely play a crucial role in gut health.
For celiac disease to exist, a person must carry one of the two celiac genes, eat gluten, and experience intestinal permeability, which can be onset by changes in the microbiome or the gut.
The gut is deeply impacted by lifestyle components, such as high-stress jobs and a lifetime of poor eating habits.
Today’s Standard American Diet (SAD) is centered on eating more processed foods loaded with sugar and salt and fewer whole foods such as fruits, vegetables, and whole grains.
The packaged food revolution also has led to greater consumption of gluten-containing foods such as bread, pasta, and baked goods, all of which can trigger celiac disease in people genetically predisposed to the condition.
Studies have shown that alterations in the gut microbiome can lead to increased intestinal permeability, which, in turn, can trigger the celiac disease genes to activate at any time.
(2) Eating Gluten Longer
Elderly patients have been eating gluten for decades, and, like a leaky faucet, the bottom finally gives out, and full-blown celiac disease ensues.
Plus, serious disorders, such as autoimmune diseases and cancer, more often appear in elderly patients who have experienced longer durations of gluten exposure in their lifetime.
A doctor may run a series of tests on an older patient for a diagnosis and surprisingly find a positive celiac disease blood test in the end.
(3) Greater Awareness
With the popularity of gluten-free food and gluten-free menus, more people than ever are aware of gluten disorders. And with greater awareness comes increased interest, scrutiny, research, and testing.
Today, many doctors routinely test for celiac disease when a patient presents with specific symptoms (see below), and more patients than ever are self-aware that their symptoms might align with celiac.
With greater awareness also comes better testing opportunities. Today, celiac disease can be diagnosed with a simple blood test.
Anyone suspecting celiac disease can even test themselves for the disorder with the invention of reliable at-home celiac disease screening tests, such as this one.
Celiac Underdiagnosed in Older Adults
Unfortunately, late-onset celiac disease is underdiagnosed in older patients, which can increase the risk of serious medical conditions and death.
One study found it took an average of nine years from the onset of symptoms to a celiac diagnosis. Another survey of elderly celiac patients found the diagnosis delay to be closer to 17 years!
One reason for delayed diagnosis is that symptoms of celiac disease are non-specific and often mistaken for other common disorders found in older people, such as acid reflux, irritable bowel syndrome (IBS), and gastroesophageal reflux disease (GERD).
As a result, doctors – and even patients – may overlook celiac disease and instead mistake their symptoms as part of getting older.
11 Signs of Late-Onset Celiac Disease
Celiac disease can present differently in patients 65+. Below are 11 signs and symptoms of undiagnosed celiac disease in older populations:
Anemia: Researchers found that anemia, micro-nutrient, and iron deficiencies are common in elderly populations with undiagnosed and untreated celiac disease.
Ataxia: Ataxia is a neurologic complication of celiac disease that can lead to a higher risk of falls in elderly patients. Elderly patients with balance issues should discuss the possibility of celiac disease with their doctors.
Calcium and Vitamin D Deficiencies: Because celiac disease impairs nutrient absorption, many elderly patients may experience decreased bone mass, bone fractures, osteopenia, and osteoporosis. Some experts recommend celiac screening for all osteoporosis patients.
Colon Cancer: One study found that adults diagnosed with celiac disease experienced an increased risk of colorectal adenomas, specifically left-sided adenomas.
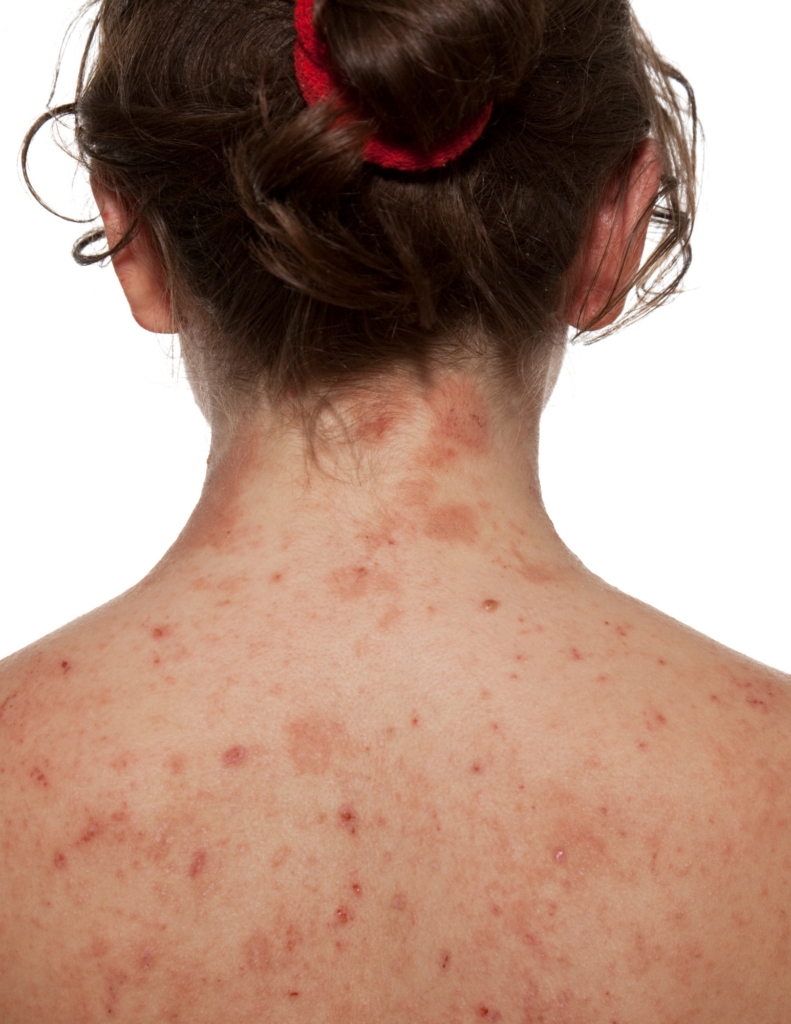
Dermatitis Herpetiformis (DH): While DH, also known as celiac rash, is a common symptom of celiac disease in all populations, the average age of presentation is 40 years old.
Gastrointestinal Symptoms: While classic gastrointestinal symptoms can still be a sign of celiac disease in elderly populations, studies suggest that diarrhea, weight loss, constipation, and abdominal pain are less common in elderly patients.
Hypothyroidism: Thyroid disorders are the most common autoimmune disorder presenting in elderly patients with celiac disease. The disorder is usually diagnosed in patients over 50.
Liver Abnormalities: Many elderly patients present abnormal liver function, known as celiac hepatitis. Studies show a gluten-free diet will likely resolve liver abnormalities present in celiac patients.
Lymphoma: Experts say elderly patients with undiagnosed or untreated celiac disease are at higher risk for intestinal lymphoma and other malignancies. The most common incidence of lymphoma occurs when celiac patients are diagnosed in the 6th, 7th, and 8th decades of life.
Neuropathy: The damaged nerves near the brain can lead to cognitive impairment and accelerated dementia in elderly patients with celiac disease. In many cases, the damage is irreversible, even with a gluten-free diet.
Refractory Celiac Disease (RCD): RCD occurs in more advanced cases of celiac disease when a patient’s symptoms don’t respond to a gluten-free diet. Approximately five percent of celiac patients develop RCD, and the median age of diagnosis is 58 years old for milder cases and 70 years old for advanced cases.
Treating Celiac Disease in Elderly Populations
The only treatment for celiac disease is a strict gluten-free diet, which can be challenging for older patients who may find it difficult to break life-long eating habits.
Some elderly patients who reside in assisted living facilities may also find it difficult to get safe gluten-free meals.
For example, a woman with celiac disease sued her retirement community for failing to provide safe gluten-free food despite being assured by the staff that they understood the seriousness of her disorder.
Specifically, she’s suing for breach of contract, negligence relating to food preparation, and negligent misrepresentation, among other claims that show the retirement community violated the Americans with Disabilities Act. Celiac disease is classified as a “disability” by the ADA.
Regardless of the difficulties, a gluten-free diet can help manage and reverse many of the ill effects of celiac disease, and making every effort to follow a strict gluten-free diet should be a top priority at any age.
The Bottom Line
The rise of late-onset celiac disease is a complex phenomenon that can be attributed to environmental factors, lifestyle changes, and greater awareness of the disorder in the 21st century.
Anyone who suspects celiac disease or experiences any symptoms noted in this article should request to be tested for celiac disease or take this at-home celiac disease screening test.
Remember, celiac disease doesn’t discriminate; it can develop at any time and at any age. Individuals need to be screened for celiac disease with the onset of symptoms irrespective of their age.
This is especially true of people with a first-degree relative with celiac disease, who experts say are at greater risk of the disorder.
Additional Reading
You might enjoy these articles, too:
I was diagnosed at 30 after the birth of my first child. The child didn’t sleep and if she was awake, she was crying. My mother-in-law told me something I was eating was bothering the baby. Fortunately my GP was an astute diagnostician who asked me several questions to which I answered yes (alternating constipation/diarrhea, bad bloating and foul gas, dry flaky skin, iron deficiency, canker sores, tooth cavities, constant and bad headaches, hypoglycemia, depression, itchy skin, allergies, and the myriad list goes on) that had been plaguing me since childhood. I also have asthma. He said I sounded like a malabsorber and sent me for a gastroscopy, sigmoidoscopy and barium enema. They were all positive. This was in 1985. We lived on the farm in northern Aberta at the time where there were no products, recipes or support. I wasn’t much of a cook and tired rapidly of trying to bake muffins without easily available ingredients which lead me to eating only meat, vegetables, fruits, potatoes and rice plus reading a lot of labels. I have thanked the stars for my diagnosis at such an early age as my father died of intestinal cancer at 46. I have since realized he must have had celiac disease. I also believe my mother’s mother had it as she died of anemia at 54.
I’m writing this tome to encourage people as I started getting colonoscopies every two years at 40. At 53 my GE did a colonoscopy, antigen blood test and gastroscopy. He said my body had healed as I had no visible signs of celiac disease and attributed it to my strict adherence to a gluten free diet. He has since retired.
I am concerned, though, because I am now 70 and I am starting to get recurring symptoms that alarm me. The itchy skin, bad bloating and gas, dark circles under my eyes, sleep problems, etc are getting really tedious after relatively good health for so long.
Can anybody point me to a resource or make suggestions on how to go forward with this?
Thanks for this website.
I was diagnosed at age 68 – about 1 1/2 years ago. My mother had celiac with “classic” symptoms. I, however, never had diarrhea, etc., that she had – and have been overweight most of my life. BUT – I had iron deficiency for years – even getting iron infusions that did not help. Also hypothyroidism, low calcium & Vitamin D, and other vitamin deficiencies because of malabsorption. After 1 1/2 years of absolutely being EXTREMELY careful and not putting a bite in my mouth that I wasn’t sure about, I can report that as of last month’s blood test, my hemoglobin is 14.8 – higher than I ever remember it!!! My Vitamin D & calcium has also improved. I feel really good – and although at first I bought a lot of gluten free processed foods, I decided in January of this year that I was going to quite eating any processed foods and stick with what is simple – and I think this is much healthier for me.
I was diagnosed two years ago at age 56. I was having serious neurological issues and non stop nausea, but no one could figure out what was going on. In a last ditch effort of desperation my Dr. ordered a huge blood panel checking for everything under the sun. That’s when we found I had Celiac disease. I’ve still got neurological issues, but at least the crippling nausea and diarrhea are gone.
Betty 4/2/23: I was diagnosed age 79/80. I grew several of my own vegetables and tried to eat a Mediterranean diet for several years. I was having problems with gas, losing weight for no reason, acid reflux, diarrhea off and on. The doctor took a blood test right away and the test came back 205. They wanted me to do a gf diet for 6 months and see what happened but my father and brother died of stomach cancer so I requested a endoscope to confirm no cancer. I’ve been on a GF diet for over a year but now I seem to be allergic to most any processed flour! I haven’t given up totally on GF pasta so I still have bloating, etc. It has been a real hit to my being able to cook like I was used to. I’m still learning. I’ve learned to soak my beans and rice before cooking and lentil beans seem to be the most gentle to my stomach. There is an app to check items in the grocery and an app to look for GF friendly restaurants. Your book was a big help getting me started to rethink how to cook.
I was diagnosed with Celiac Disease at age 60. I’d been trying to determine what was wrong with me for nearly 5 years before the diagnosis. I got so tired of poop samples – Endoscopy and a blood test with a genetic test let me know it was the real deal. I’ve been gluten free since age 60 and it is no picnic, but I am feeling much better and I don’t have uncontrollable diarrhea – I’m grateful it was not an RA diagnosis. My brother has RA – it’s the same gene causing our respective issues.
Very informative to learn the increase in older people being diagnosed with celiac; I was 78! I can count back 15 years to inconsistent gastrointestinal issues and realize I should have brought up the cramping, bloating, diarrhea much sooner with my primary care doctor than I did. At that point, my doctor had me tested for everything except Celiac because I lost 35 pounds in a t-8 month period of time. There was no connection made by my doctor to my having another autoimmune disorder (hypothyroidism diagnosis @60) which increases chances of celiac. I still deal with skin & scalp issues that cause itching. My daughter has also been diagnosed and suggested good for you gluten free to me.
I was diagnosed with celiac at age 71. I would never have known if my brother hadn’t been diagnosed and his doctor advised that all his siblings be tested too. I had no symptoms to speak of, though I had bouts of diarrhea I no longer experience. I still miss some foods, especially going out for dim sum. I would never have guessed that soy sauce contained wheat. I’ve adjusted quite well, I think, but can’t say I feel lots better as a result of being gluten free. Plus, I had hoped to lose some weight, which didn’t happen :). I really appreciate your emails and articles. Thanks.
I was diagnosed at 47 (in 1998), which was 29 years after my symptoms first started (at the age of 18). When I was finally diagnosed, I had permanent adrenal damage, and the celiac had aggravated other autoimmune diseases (rheumatoid arthritis and asthma especially). I will be forever grateful for the doctor who was determined find out what was wrong with me. That 29 years was horrid as I went from doctor to doctor, some of them accusing me of making it all up. I am still a strong reactor. I am vigilant about the gf diet. Two of my children and several nieces have also been diagnosed with celiac. Now that the family is aware, it is one of the first things that is checked when symptoms appear.
I was diagnosed at 53. I had no symptoms, but 20 years earlier I had severe anemia and was off work for 6 weeks. My iron level was 9. I was told I was drinking to much milk and the calcium was binding with iron so I wasn’t absorbing it. Limiting milk my anemia improved. But I have always been tired. No increase in energy with strict gluten free diet.
Diagnosed at age 64. It has been a rough 2+ years getting the ttg numbers to target levels. Although my daughter was diagnosed 5 years earlier I kept saying it was her father’s family that was the source of her celiac. I had no Gi symptoms and was pushed to have endoscopy due to anemia. What a shock. Upended my life.
Thank you for sharing this story with me and this community!!
I had gallbladder surgery. Afterwards, I developed an onset of maladies including b12 anemia, elevated alkaline phosphatase, increased appetite, unexplained weight loss, bloating, canker sores, cheilosis, Constipation Alternating with Diarrhea, Gastritis, Collagenous, Gastritis, Lymphocytic Gastro-Esophageal Reflux Disease (GERD), heartburn/GERD (still have), Malabsorption of Nutrients, Steatorrhea (Pale, smelly, floating stool hard to flush or sticks to toilet), Sucrose Intolerance (Gas, bloating, mucous in stool from sugar), Alopecia Areata (Patches of hair loss), Eczema, Itchy Skin Rash
Hangnail, Koilonychia (Thin nails that flatten, ends progressively turning up instead of down) and more..
I kept a list so that I’d never forget what gluten can do to me. I solved it myself because the doctor said CD was for children. My new gastroenterologist says my symptoms were more than enough to diagnose me. I did do a Gluten challenge and he diagnosed me about 5 years after the fact.
This article I’d fascinating. I was diagnosed at 52 after many years of trying to find the cause of debilitating chronic fatigue. I had had intestinal issues for so much of my life I honestly didn’t think it was abnormal so I never brought it up to my Dr. But after years of blood tests for every imaginable thing (revealing constant low wbc and platelets) I mentioned my GI issues along with the fatigue so new set of blood tests were ordered, which came back + for celiac, with extremely high antibodies. I happened to have a colonoscopy scheduled already so we added the endoscopy after my diagnosis. When I showed my GI my blood test result he laughed at the number saying the endoscopy is just a formality. No denying my diagnosis with those antibodies.
In the year since I’ve been very strict about a GF diet and was able to get my antibodies from 250 down to a 9 in about 11 months time. But learning about all the problems celiac can cause, I now suspect I’ve had it most of my life. From being underweight my whole life, tales from my parents of the constipation that I’ve had since I was a toddler, to infertility and 3 unexplained pregnancy losses in my 30’s, among other random things throughout my life that I can now trace to celiac.
I still have the fatigue and constipation so either my small intestine isn’t healed yet or I’ll need to do food allergy testing. But I can say not having the daily stomach distention and bloat is life changing. More work to be done on my health but this celiac diagnosis not only changed my current life, it answered many mysterious health questions I’ve had throughout my life
I was 67 and anemic with issues with gas bloating and loose stools when I began eating bread after not having it for approx 7 years as a life time weight watcher following a new point system. I had a small gastric bleed near the small intestine, signs of a small amount of Barret’s esophagus and had to have gallbladder removed which had 2 polyps and 19% function. Tested positive for one blood marker for celiacs and one for Crohns disease. He said no damage to small intestine. But did have 10 small cysts in liver. Opting for a new gastroenterolgist for a second opinion and to watch the Barret’s. I’ve been off gluten a diary ever since. Doing much better. I can eat some hard sharp goat cheeses but that’s all I’ve tried. I’m also staying away from most processed foods. I had 4/5 of my thyroid removed at 18 and 30 years later was diagnosed with Hashimotos disease. I’ve also been allergic to shellfish and mollusks since forever. Just learning how to eat and be healthy and continue to maintain my weight loss is quite the challenge. Hard to find physicians who are up on all the autoimmune issues.
Thanks for the great article. I was diagnosed at age 62. I’d had a lifetime of frequent GI issues and had been tested for seemingly everything. My liver enzymes had been abnormal for 3 decades, and I’ve had 2 liver biopsies that were normal. In 2020 I dropped to 100 lbs with no reason. I guess I finally found a good GI doctor who suspected Celiac, and it was confirmed. One year later, and my liver enzymes are normal. My GI symptoms are gone. BTW, I had no problem adopting and keeping a GF diet. I feel so much better! Thanks, I love your weekly emails!
Laurie
i was diagnosed at age 60. I’ve had so many red flags since childhood but the pieces were never put together until some lymphoma treatment so affected my gut that I finally went looking for answers. I have had breast cancer, currently have CLL and have had many basal cell skin cancers. I’ve had precancerous lesions in my thyroid and colon. I’m of Irish decent and have had the DNA positive test along with all the other blood work. Following a gluten free diet has helped tremendously. I think education is key. So many of my issues were never linked to Celiac. I really enjoy your page! Thank you!
One of my good friends and her husband just moved out of the neighborhood to the city to be closer to family, and she called about a month ago saying she had been diagnosed with celiac at age 77. She was so depressed because she has a large family and is a great cook. She described her symptoms and I recognized some that I had. Fortunately I had my semi-annual appointment with my naturopathic physician two days later and asked her if she thought celiac could be my problem. She immediately ordered a celiec blood test along with a food allergy and environmental allergy blood test and shared that she herself had been diagnozed with celiac. My tests came back negative, but with some underlying low-grade food allergies and she suggested eating gluten free to see if it helped me feel better. That was only a couple of weeks ago, but I’m already feeling better.
I appreciate your book which I found on line after talking with my friend, hoping I could find some information that she could read to help her on her gluten free journey. She read it right away, but is still finding it hard. I keep trying to encourage her and your book is certainly helping. Your weekly posts contain so much great information, so thank you for all you do for people with celiac and non-celiac gluten intolerance.
I was diagnosed with celiac disease at the age of 37 after my very first dose of immunotherapy(Keytruda) for cancer treatment. Pain started the very next day after infusion. EGD confirmed medication induced celiac disease. Reversed the immunotherapy treatment with steroids. Two months later blood test was positive for celiac. I get extremely ill if I eat gluten. Oncologist hopes it will go away in a year or two. I’m wondering if there are more cases because of immunotherapy!? It’s been around for only 5 years now.
I was diagnosed at 42 (in 2019) after giving up on my primary care physician. I had complained about GI symptoms for 6 years. He gave many possibilities, and I gave it time. On the 6th year, he said it sounded like IBS and I could try an antidepressant. I had been experiencing other health issues and didn’t feel right. I would ask myself, “What is wrong with me?” I had a chronic dull sinus headache 24/7/365 for years. I had been diagnosed with toenail fungus in 2015, told it was likely a weakened immune system. I had an episode of hair loss in 2016, dermatologist said, “Sometimes that just happens.” I had a myriad of symptoms that I couldn’t figure out or tie to anything and I didn’t know what to do about them. I had heart palpitations (that I first started experiencing when pregnant with my daughter in 2010), the headaches, bloating, very strange stools that I didn’t think of as diarrhea, muscle cramps, shortness of breath, rashes that would come and go inside the creases of my elbows, sexual activity was painful and I would bleed after, weakness and fatigue. I spoke with my doctor about some of them, hormones were always blamed. The only test run was my thyroid when my hair was falling out. It was a low-normal range so nothing more was done. When I felt like I was dying a slow death, I started with the most consistent symptom and took myself to a GI and asked that tests be run. Even though I was diagnosed at 42, I’ve had a lifetime of health issues that could have been celiac at a time that I didn’t have GI symptoms. I believe it’s possible that I’ve had celiac since a horrible case of chicken pox at 17 years old. That’s when strange health issues started happening. I will screen my kids every 5 years. I won’t wait for them to have symptoms. I believe public should be routinely screened.
I was diagnosed at the age of 84 yrs. Up to that time I was in excellent health (except for arthritis) and could eat everything without consequence. I had been on Synthroid for 61 years; levels checked regularly.
Then my husband after years of my at-home care. Shortly later bouts of diarrhea disabled me. Blood tests for gluten allergy were neither positive or negative. A colonoscopy was negative. No doctor thought of gastroendoscopy.
I started eating a gluten-free diet which stopped the diarrhea. now, 3 years later, it will return if I accidentally ingest a small amount of gluten.
I can only conclude there was an emotional conponent which sparked the onset.
Thanks for the article, Jenny. I was diagnosed May 2022 at age 52 after a year of symptoms, none of which were GI related. SEVERE itching and fatigue were my main issues although I also have a gluten rash on my neck and chest. When I first went to the doctor for the itching, my doctor told me it was a yeast infection! I knew that was not the issue but couldn’t convince the doctor. Three yeast infection treatments later, a biopsy and multiple blood tests (I was told they tested for autoimmune) revealed nothing. I changed my doctor which eventually led to a referral to a dermatologist – a new biopsy and blood work and finally a diagnosis. I have another autoimmune disease (diagnosed at age 27), hypothyroidism (diagnosed in my 40’s) and have had migraine headaches since age 16. I am learning a whole new lifestyle and still struggle with the loss but, overall, I feel much better. I find the GF diet incredibly hard to follow – not that I am unwilling, but that gluten is hidden in unexpected places and can be so easily cross-contaminated at restaurants. Thanks, Jenny for helping me navigate this new world.
I was diagnosed at the age of 70. My granddaughter was diagnosed at 5 with small intestine byopsy. At that time I was not having any changes in my gastrointestinal symptoms. Although I have spent my whole life dealing with bouts of nausea and constipation which had been accredited to food allergies. I had 23 and me genetic testing done for “the fun of it” and came up with both celiac markers. My doctor ran one blood test which came up negative. About a year later I started having diarrhea symptoms which improved when I stayed off gluten. I then went and had the gluten challenge endoscopy, but the doctor who did the test was convinced I did not have celiac and only took two samples to byopsy which came back negative. My primary care physician and I decided it was not worth any more testing if staying off gluten helps. I have now been gluten free for 5 years and I can really tell if I have gotten exposed.
I was diagnosed at age 66 – 4 years ago. I started having some stomach issues and went my gastro doctor who asked me if celiac ran in my family – I said no. She ran the celiac blood test and it was positive. Had a colonoscopy a week later and no damage was found. From symptoms to diagnosis was a month or two so I feel very lucky that my gastro doctor (who I had only seen twice before for colonoscopies) knows a lot about celiac. I feel 100% fine while eating gluten free. My hardest part is going out to eat. Luckily I live in a big city (Atlanta) and I can pretty much find something to eat that’s gluten free. Celiac can be a real pain so I am glad I did not get it as a child. I feel for them….
Hi, I was diagnosed at age 53. I had been losing my hair, had severely low ferritin, GI issues, joint pain, fatigue, etc for many years. These symptoms were blamed on many things – “getting older” is what I heard mostly from multiple doctors. I was diagnosed with Hashimoto’s and Fibromyalgia/Chronic Fatigue Syndrome 16+ years previous. Then I was having severe gallbladder disease symptoms a couple of years ago. The GI decided to rule out stomach ulcer and I had an endoscopy where they accidentally found I was positive for Celiac Disease. All those years no one even considered it. Once I was eating gluten free I was able to stop taking most of the medications I was on for Fibro. I really believe that the medical community is very ignorant on the symptoms/diagnosis of Celiac disease. My GI told me once I stop eating gluten no follow up is warranted with him. No yearly checkups necessary. In fact, I had a family doctor ask me “how much gluten I could get away with eating?”. Do I “get symptoms after eating gluten?” I couldn’t believe it. She did not realize that even if you don’t get symptoms that there is still damage to the gut. I believe my Mom had celiac disease too. She had so many issues with her gut over the years. No one ever checked. You have to be your own best advocate out there. If a doctor doesn’t listen to you or tells you something that doesn’t seem right – get another opinion. Best health to all!
Thank you for this post.
I was diagnosed at age 46, genetic markers from both parents and reaction to gluten was 3x the size of the chart. Started GF diet and my gut took almost 2 yrs to heal to a point where foods could digest better. Eating plain veggies would cause a reaction. If you get diagnosed and start eating GF, be patient. Your body needs to adjust and heal.
7 yrs later and I have learned (the hard way) that my body cannot digest certain gluten free foods: dairy, corn, oats, russet potatoes (sweet potatoes are ok) and soy. Getting diagnosed later in life and possibly 4+ decades of damage by eating gluten permanently changed my system.
Great content here! Thank you for everything you share.
Thank you for sharing your story and for your kind words!
Hi Jenny, thanks so much for this great article! I don’t feel so abnormal or alone now. I was diagnosed at 62. I had no extreme abdominal issues; the red flag that led to my eventual diagnosis was a consistent slight elevation of my liver enzymes which led to an appointment with a gastroenterologist. He wasn’t terribly concerned but decided at the last minute of my visit to order up a more complete liver panel which must have included the test for Celiac. I never heard from those tests figuring no news is good news. That was until my dermatologist ordered bloodwork to determine the cause of recurring mouth sores and lip discoloration. She saw the iron deficiencies and felt there may be a connection and instructed me to follow up with the gastroenterologist. The Celiac connection was there in the bloodwork which led to the endoscopy and my eventual diagnosis! He sent me out the door saying: “Don’t eat wheat, barley or rye and here’s a referral to a dietician.” The dietician’s specialty was diabetes and she knew nothing about Celiac above what I had already found online. Thankfully, I found your wonderful book!! That got me on the right course for sure. It was hard since I had no abdominal issues. I know that sounds funny, but I was always paranoid that I may be getting gluten via cross-contact without knowing. I do suffer with Dermatitis Herpetiformis. I had small breakout for years not knowing what it was. After being on a gluten free diet for about a year, I had a bad DH breakout which was very confusing. I took an online course with Maya Rose and she told me that wasn’t unusual. She suggested getting my dermatologist involved. I’ve been on dapsone now for about 6 months and it seems to be helping.
Sorry this is so long! I enjoyed reading the other posts. Celiac Disease is quite a journey! I think the blood test should be something that doctors do routinely to prevent the damage that it can do!
Thanks again for your wonderful book, weekly blogs and amazing website! I appreciate you!!
I’m glad you figured it out!
So interesting. I hope you’re feeling better now.
Thank you for sharing your story.
Wow I’m so glad one doctor thought to test you for celiac!!
I was diagnosed at about age 40. The acute symptoms that I began having were chest pain and tightness and inability to keep any foods in. I went to the hospital 3 times because it felt like something was seriously wrong with my heart. They ran a stress test and a million other tests, but nothing was coming up at all. I ended up getting a new primary doctor who said, “let’s just add the Celiac panel here even though there is no family history. ” That is what it was – Celiac. The antibody count was through the roof – he could not believe it. The endoscopy confirmed it.
My husband turned 60 and small things started to ail him, dry cracked heels for one we live in Italy and he is out in the 3 acres of garden most of the day so more TLC and moisturizer, then he started suffering what what we thought were allergies to the local flora so added antihistamines, then he was over heating and disclosed he wasn’t sweating, this started all sorts of alarm bells but I was told I was fussing and he was fine. Then the stomach cramps, runs, feeling weak, was cold despite heating flat out and 5 layers and the weight loss at which point I threatened an ambulance or he saw a Dr, who was marvelous and despite being in the midst of the Covid chaos got him though the tests, scans, etc for the diagnosis at the age of 63 and confirmed in just over 1 year.
He has class 3 Celiacs , Horishimas throat from reflux, dysfunctional thyroid – it doesn’t function any more as it was used up trying the make up for the gut reactions putting his system out of balance, and osteoporosis, but pills, supplements and relying on blog sites to relearn how to cook to keep him well means he’s almost back to the way he was now at 66, before it all unraveled.
Here in Italy 1% of the population have been certified with this disease and more suffer a gluten issue and being a country that lives on bread, pasta and pizza it’s a devastating diagnosis but the government give a monthly allowance to help cover the extra costs for GF products and many shops, cafe’s and restaurants are aware and will offer GF foods especially if forewarned.
I broke out with blisters on my elbows the day after spinal fusion surgery in march 2020. It took 2 1/2 years to get diagnosed with Dermatitis Herpetiformis after a biopsy, and shortly duodenal biopsies confirmed the diagnosis in May 2022 at age 70. I was diagnosed with graves disease, another autoimmune condition at age 35 after a C section when my daughter was born. I developed arthritis in my 50s and have deficiencies in vitamin D and B. Pretty sure my processed food diet through most of my life played a huge role. I am now on a diet free of gluten, and I eat predominantly fruits, veggies, fish, lean meat, and healthy fats. I have also lost weight. I have also been diagnosed with some neuropathy, and have had migraines since my 30s.
I was told by my gastroenterologist that I was too old to just develop celiac now(70 years). Fortunately my endocrinologist (my thyroid was going between Hashimoto’s and Grave’s) had ordered a celiac panel and the results came in the day after my gastroenterologist appointment, positive ! Of course my gastro was happy to do an endoscopy on me which also confirmed celiac. Her nurse told me don’t eat gluten and that was it. No follow up. I’m looking for a new gastro.
Please remind people to continue eating gluten-containing food until they’ve been tested for celiac disease. Of course, getting a DNA test for the genetic variants would be a good starting point, as well. Since you can’t develop celiac disease unless you have one or both of those variants, if you don’t have either one, that would eliminate celiac disease and could point you in a different direction for further testing of symptoms.
Yes the at home tests are a great first start and accurate. Regardless of the outcome, discuss the results with your dr.
Fascinating! Thank you for this information. I have ruled out gluten since I was in my late 30’s. I had an astute doctor. I am now in my early 70’s. Are you confident that the self testing works?