
This post features the 10 most common signs and symptoms of celiac disease (also known as coeliac disease) and contains affiliate links. Please consult your doctor if you suspect you have celiac disease and read my disclosures and disclaimers.
In this article, I discuss the 10 MOST common signs and symptoms of celiac disease to help you understand whether or not celiac disease might be at play in your body.
Celiac disease is an autoimmune disease where a patient’s immune system becomes confused and attacks the healthy tissue surrounding the small intestine.
People with celiac disease are typically diagnosed via a simple blood test and/or biopsy of the small intestine, where a doctor looks for flattened and damaged microvilli. The villi are the finger-like follicles surrounding the small intestine responsible for nutrient absorption and distribution.
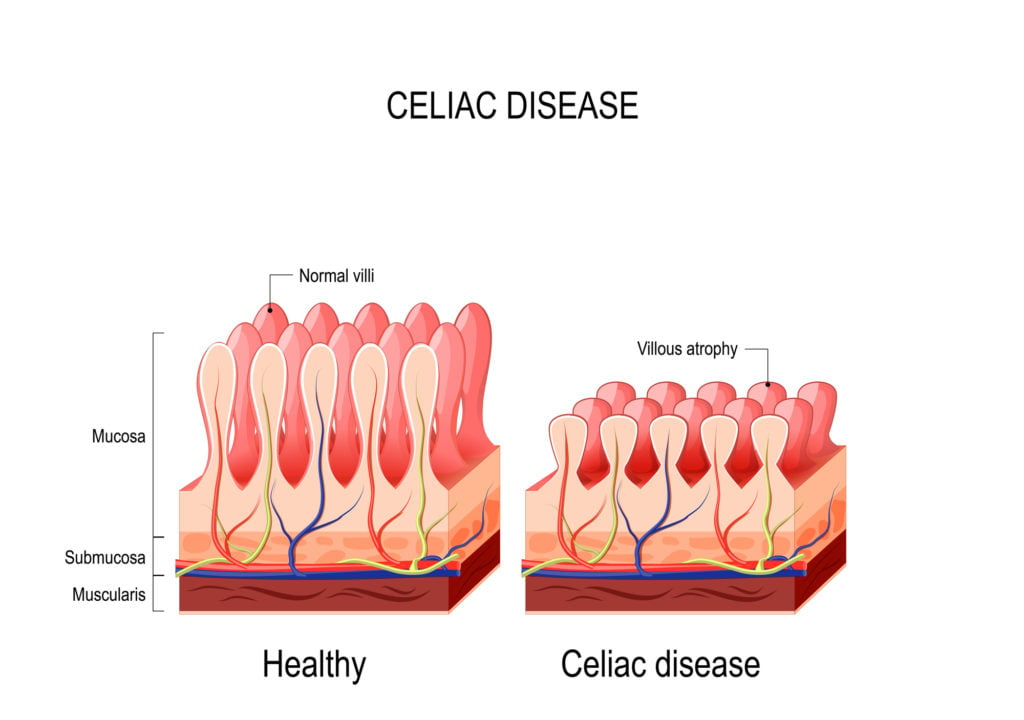
When the small intestine is damaged and inflamed, celiac disease manifests itself in a slew of different ways throughout your body.
In fact, celiac disease can rear its ugly head via one or of the dozens of different documented symptoms, many of which I’ll cover in this article.
Unfortunately, celiac disease is an underdiagnosed disorder, and 78 percent of people with celiac disease don’t even know they have it because it’s so difficult to detect and diagnose.
Related Reading: What is Celiac Disease?
For example, if your joints hurt, you don’t automatically think to get tested for celiac disease, nor would you connect a simple canker sore in your mouth to celiac disease.
Perhaps, however, these innocuous symptoms are clues from your body telling you to dig deeper to investigate the root cause of how joint pain, or an innocent canker sore, came to be. Maybe there’s more to those symptoms than meets the eye.
The 10 MOST Common Symptoms of Celiac Disease
The following list includes the 10 most common signs and symptoms of celiac disease. Please be sure to discuss any of these symptoms with your doctor.
(1) Digestive Disorders
Because celiac disease is a disorder of the digestive system, many people experience a slew of digestive disorders signaling something isn’t right in their bodies.
Severe bloating, diarrhea, constipation, and excessive, uncomfortable gas are just a few of the digestive symptoms that could signal you have celiac disease.
The good news is, however, that most of these uncomfortable and embarrassing symptoms clear upon implementation of a gluten-free diet, which is the only treatment available to people with celiac disease.
(2) Fatigue
When you have celiac disease, your body’s ability to properly absorb and distribute nutrients to where they need to be in your body becomes impaired. This is why many celiac patients feel chronically fatigued.
You may be eating plenty of healthy foods, but if you have celiac disease, your small intestine cannot properly absorb or distribute those nutrients. This might leave you feeling nutrient deprived and, therefore, fatigued.
Additionally, some celiac disease patients are underweight, often due to the lack of nutrient absorption. Conversely, some celiac disease patients are overweight as they might be overeating in order to fully feel nourished.
(3) Skin Disorders
The skin is the largest organ in your body and is often a window to what might be going on inside of you.
There are several skin conditions related to an abnormal immune system response to gluten, including the following.
Dermatitis Herpetiformis (DH): DH is a chronic inflammatory disease of the skin that appears in the form of lesions that burn and itch (DH is sometimes called celiac rash). DH is often diagnosed (or misdiagnosed) as eczema.
DH is an autoimmune disease where blisters appear on the elbows, knees, buttocks, back and/or scalp. The bumps are usually symmetrical, and skin blisters often appear on the same spot in both elbows, for example.
Only about 20% of people with DH have intestinal symptoms commonly associated with celiac disease; however, they experience the same intestinal damage consistent with celiac disease.
People with DH must follow a strict gluten-free diet like those with celiac disease.
Keratosis Pilaris: This condition, also called chicken skin, is a chronic skin condition where raised, hard bumps appear on the skin. Research indicates those with keratosis pilaris may also have a fatty acid and vitamin A deficiency due to impaired absorption of nutrients.
Acne and dry skin: Acne, dry skin, and dry mouth have also been linked to poor nutrient absorption, which is consistent in people with celiac disease and other gluten disorders.
(4) Cold and Mouth Sores
Celiac disease can also manifest itself in the mouth. In fact, people with celiac disease may experience more cavities, canker sores, mouth ulcers, broken teeth, and tooth decay than those without.
One study found that enamel defects are common in adults with celiac disease and that observation of these effects is another way to potentially diagnose celiac disease.
Another study found that a pattern of enamel defects and oral aphthae (small ulcers appearing in the mouth or tongue) are common findings in celiac disease, thus making the dentist an integral part of the celiac disease diagnostic team.
Geographic tongue, for example, is a benign inflammatory condition where an ulcer or sore patch appears on your tongue. One study showed an increased prevalence of geographic tongue in patients with celiac disease.

(5) Brain Disorders
There are a variety of psychological manifestations of celiac disease, such as anxiety, depression, aggressive behaviors, ADHD, and sleep disorders.
A gluten-free diet has been shown to help combat many of the symptoms associated with these diagnoses, albeit a lot of information is still unknown.
One well-documented case of psychiatric behaviors improving with a gluten-free diet is of an anonymous patient admitted to a psychiatric ward due to suicidal and agitated behaviors.
The patient was unresponsive to antidepressants and other medications and therapies. An extensive diagnostic study showed the patient had celiac disease. The patient improved significantly once he started a gluten-free diet.
A lot of patients managing ADHD are often nutrient deficient (particularly in fatty acids and Vitamin A), and once those deficiencies are addressed, the patients significantly improve, according to Dr. Mark Hyman in his book, The UltraMind Solution.
Jennifer Esposito writes in her book, Jennifer’s Way, that she suffered from “mental disorders” that stemmed from undiagnosed celiac disease.
Her doctor thought she was crazy, but she knew something was wrong with her. She was finally validated when she found out she had celiac disease, which was the root cause of her anxiety.
Celiac disease may also be more likely to be found in children with behavior issues.
One study, which tracked 8,676 infants deemed at high risk for celiac disease, had mothers assess their child’s behavior at ages 3.5 years and 4.5 years. If a child was found to have celiac disease, the researchers would revisit the earlier behavior scores.
The mothers unaware of whether or not their child had celiac disease had reported that their children experienced a greater level of anxiety, depression, aggression, and sleep problems than the mothers who knew their child’s diagnosis or the mothers of children without celiac disease
(6) Failure to Thrive and Short Stature
A child of short stature or who is failing to thrive is a strong sign that the child might have celiac disease. Studies confirm this correlation too.
A child who isn’t growing properly or failing to meet milestones should be tested for celiac disease. This is absolutely one of the key signs and symptoms of celiac disease. Read: 10 Signs of Celiac Disease in Kids.
(7) Bone Density Issues
An issue with gluten can also manifest itself in the form of bone problems.
Osteoporosis, recurrent bone fractures in the limbs, joint pain, arthritis, and swollen joints are often signs of celiac disease.
If you have bone density issues ranging from osteopenia (mild) to osteoporosis (severe), you may have trouble absorbing nutrients and suffer from celiac disease.
(8) Migraines
Food intolerances are often the root cause of chronic inflammation, including migraines.
Dr. Mark Hyman says wheat and gluten are among the biggest triggers of headaches and migraines. He also suggests other foods, like corn, dairy, eggs, and yeast, can trigger migraines and headaches.
Furthermore, researchers from Columbia University in New York found a greater incidence of headaches and severe headaches in celiac patients.
One study published in 2021 also found a higher prevalence of migraines in patients with celiac disease when compared with healthy controls.
(9) Autoimmune Disease
Having one autoimmune disease puts you at a 25 percent greater likelihood of accumulating another autoimmune disease.
Therefore, if you already have an autoimmune disease, you are at risk of getting celiac disease or another one of the hundreds of classified autoimmune diseases, including but not limited to:
- Addison’s disease
- Alopecia
- Crohn’s disease
- Graves’ disease
- Hashimoto’s thyroiditis
- Lupus
- Multiple Sclerosis
- Psoriasis
- Rheumatoid arthritis
- Scleroderma
- Type 1 Diabetes
- Ulcerative colitis
(10) Infertility
While studies are inconsistent, incomplete, or non-conclusive about whether or not gluten disorders are related to fertility issues, there is evidence suggesting that celiac disease is known to cause adverse reproductive consequences, including infertility and recurrent pregnancy loss.
One study suggested that celiac disease is related to infertility in 4-8 percent of patients.
Reproductive problems such as infertility and irregular menstrual cycles are often connected to gluten intolerance as well.
Experts say that inflammation caused by gluten puts stress on the adrenal glands, which then malfunction and upset the balance of the endocrine system.
Another study in New York of patients with unexplained infertility found that 6 percent of the patients had confirmed cases of previously undiagnosed celiac disease.
Another study found the incidence of miscarriage and premature birth is higher in those with celiac disease than in the general population. Some experts say this may be due to complications related to nutritional deficiencies prevalent in those with undiagnosed celiac disease.
Elisabeth Hasselbeck talks about her struggle with infertility openly in her book, The G Free Diet. When she realized she had celiac disease, and once she began a gluten-free diet, she was finally able to conceive a baby.
Nearly 15 percent of the 2,000 women with celiac disease who took part in the Canadian Celiac Health Survey said they had difficulty conceiving, and nearly one-third of the participants had miscarriages.
(11) Celiac Eye Symptoms
I added an 11th symptom, as I had been getting a lot of questions related to eye health and celiac disease.
I’ve learned that celiac disease can manifest itself through various ophthalmic manifestations as well.
Symptoms affecting the eye are typically due to malabsorption issues (remember, unmanaged celiac disease impairs your ability to properly absorb nutrients) and include disorders such as retinopathy, cataracts, and dry eye.
Other eye manifestations are attributed to immune system dysfunction and can manifest in disorders such as orbital myositis and uveitis (inflammation in the eye).
This study discusses the link between celiac disease and these various eye conditions in greater detail.
Next Steps
If, after reading this article, you suspect you have celiac disease, please consult your doctor about getting tested for celiac disease. You can also test yourself for celiac disease at home with this at-home celiac disease screening kit.
Remember, celiac disease – and other gluten disorders – can manifest itself in more than just via digestive woes. It can cause nervous system disorders, bone loss, joint pain, skin issues, and even infertility.
Please discuss any symptoms with your doctor, and whatever you do, don’t go gluten-free until you rule out celiac disease. You must be eating gluten in order for a celiac test to be accurate. Read: STOP! Don’t Go Gluten-Free Until You Read This Article.
One symptom you didn’t mention is chronic hypoglycemia. It made my life hell for years but vanished as soon as I went gluten-free.